Statin Myopathy Risk Assessment Tool
Understand Your Risk
This tool estimates your risk of developing statin-induced muscle pain based on factors discussed in the article. Your results will help guide conversations with your healthcare provider.
Your Risk Assessment
Recommended Actions
More than 39 million Americans take statins every year to lower cholesterol and reduce heart attack risk. But for a significant number of them, the benefits come with a painful trade-off: unexplained muscle pain, weakness, or cramps that don’t go away. This isn’t just "getting older" or "being out of shape." It’s a real, measurable condition called statin-induced myopathy-and it’s more common than most doctors admit.
What Exactly Is Statin-Induced Myopathy?
Statin myopathy isn’t one single problem. It’s a spectrum. At the mild end, you might feel sore after walking up stairs. At the severe end, you can’t lift your arm, climb stairs, or even stand up from a chair without help. The most serious form, rhabdomyolysis, is rare-less than 1 in 1,000 users-but it can cause kidney failure.
The real issue? Most people don’t realize their muscle pain is linked to their statin. Symptoms usually show up within the first six months of starting the drug. You might think it’s from a new workout, aging, or just stress. But if the pain started after you began taking atorvastatin, simvastatin, or rosuvastatin, it’s worth considering.
Studies show about 10% to 30% of statin users report muscle symptoms. That’s 1 in 10 to 1 in 3 people. And while only 0.1% to 0.5% develop true myopathy with elevated creatine kinase (CK) levels, those numbers don’t capture the quiet suffering-people who quit their meds because the pain was too much, or who reduced doses to cope.
Why Do Statins Hurt Your Muscles?
For years, doctors blamed CoQ10 depletion. It made sense: statins block the same pathway that makes cholesterol-and CoQ10, a compound your muscles need for energy. But new research shows that’s only part of the story.
Here’s what’s really happening inside your muscle cells:
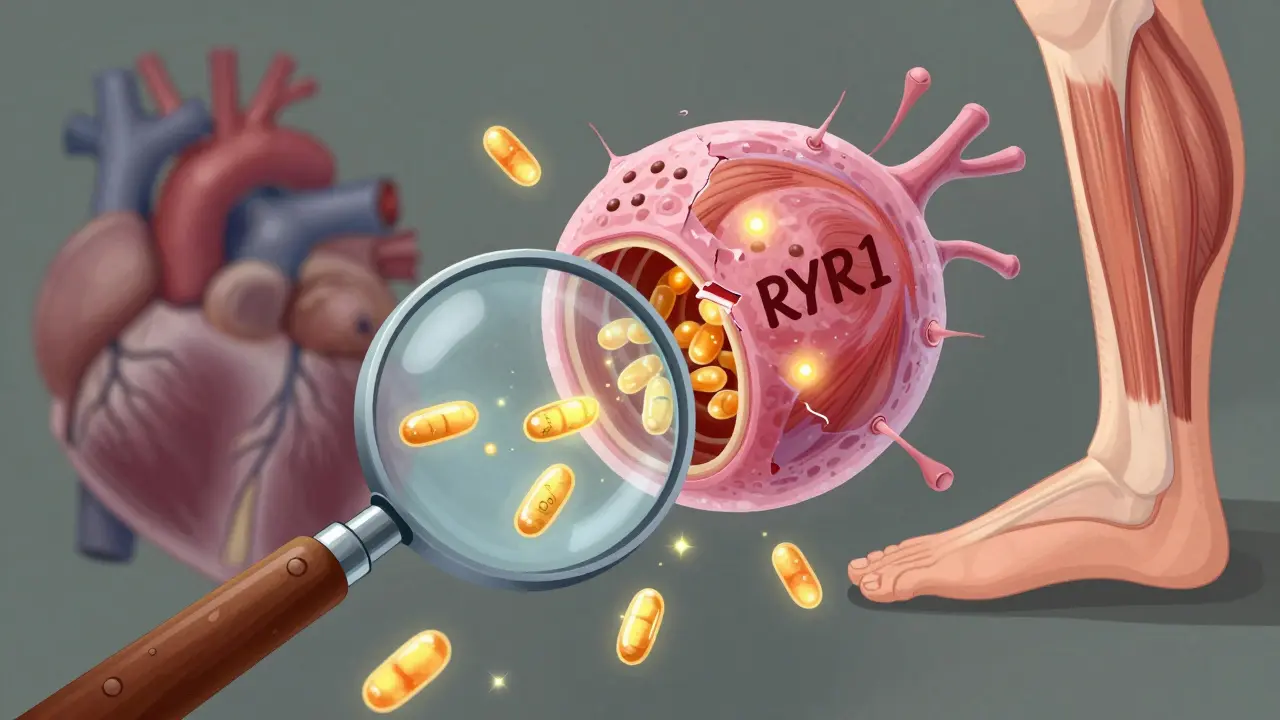
- Calcium leaks: Statins cause a protein called FKBP12 to fall off the ryanodine receptor (RyR1), a gate in your muscle cells that controls calcium flow. When it’s loose, calcium spills out uncontrollably. In human muscle biopsies, this leak increased by 2.3 times. That constant calcium surge triggers muscle cell damage and death.
- Energy crisis: Statins cut CoQ10 levels in muscle tissue by about 40% after just four weeks. Without enough CoQ10, mitochondria can’t produce energy efficiently. This leads to fatigue and oxidative stress-your muscles are basically running on fumes.
- Broken signaling: Statins also block the production of isoprenoids like farnesyl pyrophosphate and geranylgeranyl pyrophosphate. These molecules help anchor key proteins to cell membranes. When they’re missing, muscle repair and communication systems start to fail.
- Autoimmune twist: In 5% to 10% of persistent cases, your body starts making antibodies against HMG-CoA reductase-the very enzyme statins target. This is called anti-HMGCR myositis. It’s rare (affecting about 0.02% of users), but once it happens, stopping the statin isn’t enough. You need immunosuppressants like prednisone and methotrexate.
These mechanisms don’t happen in the heart. That’s why statins protect your heart but damage your skeletal muscles. It’s not a mistake-it’s a biological quirk.
Who’s Most at Risk?
Not everyone gets muscle pain on statins. But certain factors raise your odds:
- Age: Over 65? Your muscles are less resilient.
- Gender: Women report symptoms more often, though the reason isn’t fully clear.
- Dose: Higher doses = higher risk. Simvastatin 80 mg has the highest rate of myopathy.
- Drug interactions: Taking statins with fibrates, certain antibiotics (like erythromycin), or grapefruit juice can spike statin levels in your blood.
- Genetics: Some people have gene variants (like SLCO1B1) that make it harder for their liver to clear statins, leading to higher muscle exposure.
- Sedentary lifestyle: People who don’t move regularly are more likely to develop symptoms.
And here’s the kicker: you can have normal CK levels and still have muscle pain. CK tests don’t catch everything. That’s why many doctors miss it.
What Should You Do If You Have Muscle Pain?
If you’re on a statin and feel unexplained muscle soreness, don’t just tough it out. Don’t quit cold turkey either. Follow this step-by-step approach:
- Track your symptoms. When did they start? Do they get worse after activity? Do they improve on rest days? Keep a journal.
- Get your CK checked. A simple blood test can show if muscle damage is happening. But remember: normal CK doesn’t rule out pain.
- Do a washout. Stop the statin for 4 weeks. If your pain fades, it’s likely the drug. If it doesn’t, look for other causes.
- Rechallenge carefully. Try switching to a different statin-rosuvastatin or pravastatin tend to be better tolerated. Or lower the dose. About 65% of people can tolerate a reduced dose.
- Consider supplements. CoQ10 at 200 mg daily helped 35% of patients in clinical trials. Some report better results with ubiquinol, the active form.
- Move more. A 2021 Mayo Clinic study found that patients who did 150 minutes of moderate exercise per week (like brisk walking) had 41% fewer symptoms. Exercise seems to help stabilize the calcium leak.
- Look at alternatives. If statins keep causing pain, ezetimibe or PCSK9 inhibitors (like evolocumab) can lower LDL without the same muscle risks. Evolocumab’s muscle side effect rate is only 3.7%-lower than placebo.

What’s on the Horizon?
Researchers aren’t giving up. New drugs are being tested specifically to fix the calcium leak:
- S107: A drug that stabilizes RyR1. In a 2023 trial, it cut muscle symptoms by 52% and calcium sparks by 65%.
- STT-101 and STT-202: Next-gen statins designed to stay out of muscle tissue. In animal studies, they reach 70% less muscle tissue than atorvastatin-while still lowering cholesterol just as well.
And here’s good news: combining moderate exercise with CoQ10 supplementation resolved symptoms in 80% of patients in a 2024 study. That’s higher than either one alone.
Why This Matters
Statin myopathy isn’t just about discomfort. It’s about survival. When people stop their statins because of muscle pain, their risk of heart attack or stroke goes up by 25%. That’s why the American College of Cardiology now says: don’t give up on statins-find a way to keep taking them.
Doctors are getting better at this. In 2023, 78% of cardiologists started talking about muscle risks before prescribing statins. That’s progress.
But you still need to be your own advocate. If you feel muscle pain after starting a statin, speak up. Ask about CoQ10. Ask about exercise. Ask about alternatives. You don’t have to choose between heart health and muscle function. The science now shows there’s a better way.
Can statin muscle pain go away on its own?
Yes, in most cases. If the pain is caused by the statin, symptoms typically improve within 1 to 4 weeks after stopping the drug. About 80% of people see relief after a 4-week washout period. But if the pain persists after stopping, it may be due to another cause-or in rare cases, an autoimmune reaction that needs treatment.
Is CoQ10 supplementation proven to help with statin muscle pain?
Yes, but not for everyone. Clinical trials show that taking 200 mg of CoQ10 daily reduces muscle pain in about 35% of statin users. One study found that people who took CoQ10 reported less fatigue and improved physical function. It works best when combined with moderate exercise. The effect is likely due to restoring energy production in muscle cells, not just reducing oxidative stress.
Can you take statins again after having muscle pain?
Many people can. About 40% of those who stopped statins due to muscle pain tolerate a different statin. Another 65% can handle a lower dose. Switching from simvastatin to pravastatin or rosuvastatin often helps. Always restart under medical supervision. If pain returns, it’s a sign your body doesn’t tolerate statins well-and alternatives should be explored.
Do all statins cause muscle pain equally?
No. Simvastatin and lovastatin have the highest risk, especially at high doses. Atorvastatin carries moderate risk. Rosuvastatin and pravastatin are generally better tolerated. Fluvastatin and pitavastatin appear to have the lowest rates of muscle-related side effects. The difference comes down to how each statin is metabolized and how much enters muscle tissue.
Is exercise safe if you have statin myopathy?
Yes-and it’s recommended. Contrary to old advice, moderate exercise like walking, cycling, or swimming doesn’t worsen statin myopathy. In fact, studies show it helps. A 2023 JUPITER subanalysis found exercisers had 32% lower creatine kinase levels and 41% fewer symptoms than sedentary users. Exercise appears to stabilize the calcium leak in muscle cells. Aim for 150 minutes a week of moderate activity.
What are the alternatives to statins if muscle pain persists?
Ezetimibe lowers LDL cholesterol by about 20% and has minimal muscle side effects. PCSK9 inhibitors like evolocumab and alirocumab reduce LDL by 50-60% and have muscle adverse event rates similar to placebo (around 3.7%). Bempedoic acid is another option-it lowers LDL and has a lower risk of muscle pain than statins. These are typically used when statins aren’t tolerated, especially in high-risk patients.
Can statin myopathy turn into a permanent condition?
In most cases, no. Once the statin is stopped and the body clears it, muscle function returns. But in the rare autoimmune form (anti-HMGCR myositis), muscle damage can persist or even worsen without treatment. This form requires immunosuppressive drugs like prednisone and methotrexate. If muscle weakness lasts more than 8 weeks after stopping statins, see a specialist-this could be autoimmune myositis.




10 Comments
Just wanted to say I’ve been on rosuvastatin for 3 years and started having leg cramps last winter. Thought it was just aging-turns out, it was the statin. I switched to pravastatin, cut my dose in half, and started taking ubiquinol. My legs feel like they belong to me again. No more midnight toe-spasms. Also, walking 20 mins a day made a bigger difference than I expected. Thanks for the clear breakdown.
It’s fascinating how the body’s biochemistry can be both the source of salvation and the architect of suffering. Statins block HMG-CoA reductase to reduce LDL-noble intent-but in doing so, they inadvertently disrupt the very machinery that powers skeletal muscle. The calcium leak via RyR1 destabilization? That’s not a side effect. It’s a systemic collateral. We treat symptoms, but rarely the mechanism. We need targeted stabilizers, not just substitutions.
So... statins make your muscles leak calcium like a busted faucet, and now we’re supposed to take CoQ10 and walk? Cool. Cool cool cool. I’m just here wondering why we didn’t figure this out before we gave these things to 39 million people. Also, ‘exercise helps’ is the medical equivalent of ‘just be happy.’
While I appreciate the thoroughness of this post, I must emphasize that the clinical evidence supporting CoQ10 supplementation remains inconclusive. The majority of randomized controlled trials show negligible effect sizes. Furthermore, the notion that ‘exercise stabilizes calcium leaks’ is speculative at best. Without peer-reviewed mechanistic studies in humans, this reads more like anecdotal extrapolation than evidence-based medicine.
Y’all are overthinking this. I was on simvastatin 80mg, felt like my legs were full of wet cement. Stopped it. Did 30 mins of walking every day. Took 200mg ubiquinol. Within 3 weeks? Back to normal. No drama. No blood tests needed. My doc was like ‘uh huh, yeah that happens.’ So yeah. Move. Supplement. Switch statins if needed. Simple as that. 🙌
bro i swear statins are like that one friend who says they care but always leaves you hanging. i was on atorvastatin and my thighs felt like they’d been run over by a semi. i tried coq10, it helped a lil, but the real win? switching to pravastatin. felt like my body got a software update. also, grapefruit juice? nope. not even a splash. that stuff is basically a statin turbocharger. stay safe out there.
THIS IS A PHARMA COVER-UP. They know statins cause muscle degradation. They know the calcium leak. They know the autoimmune angle. But they won’t admit it because statins are the #1 revenue generator in cardiology. The ‘exercise and CoQ10’ advice? A distraction. The real solution? Ban statins. Or at least require mandatory muscle biopsies before prescribing. This isn’t medicine-it’s exploitation.
From a pharmacokinetic standpoint, the SLCO1B1 polymorphism significantly elevates systemic statin exposure, particularly for simvastatin and atorvastatin. The resultant myopathy is not merely a pharmacodynamic artifact but a direct consequence of altered hepatic uptake and subsequent myocellular accumulation. The proposed mechanisms-RyR1 destabilization, isoprenoid depletion, and mitochondrial dysfunction-are mechanistically coherent and supported by in vitro and murine models. However, clinical translation remains heterogeneous due to epigenetic and environmental modulators.
OMG YES. I started statins last year and thought I was just out of shape. Then I started walking every day and took CoQ10-and my energy came back! I didn’t even realize how tired I was until I wasn’t tired anymore. Also, switching from simvastatin to rosuvastatin was a game-changer. You’re not weak if this happens. Your body’s just telling you something. 💪✨
Let’s be real. If you’re taking statins because you’re scared of a heart attack, you’re probably eating too much sugar and sitting on your butt all day. This whole muscle pain thing is just karma for living like a couch potato. Take responsibility. Stop blaming the drug. And if you’re too lazy to walk? Then maybe you shouldn’t be on a statin in the first place.